For early-onset colorectal cancer, researchers have found that American blacks, Native Americans, and Americans of Asian and Pacific Islander descent are 1.5 to two times as likely as older people of the same ethnicity to develop the disease.
Their analysis, using the U.S. Surveillance, Epidemiology, and End Results program database, also showed that median survival was nearly five years shorter for nonwhite patients with CRC (94 months) than white patients (153 months).
“Nonwhite races overall had poor survival across all age groups,” reported Dhruvika Mukhija, MD, a fellow in hematology/oncology at Northwestern University, in Chicago, who conducted this study with Sajan Nagpal, MBBS, an assistant professor of medicine at the University of Chicago.
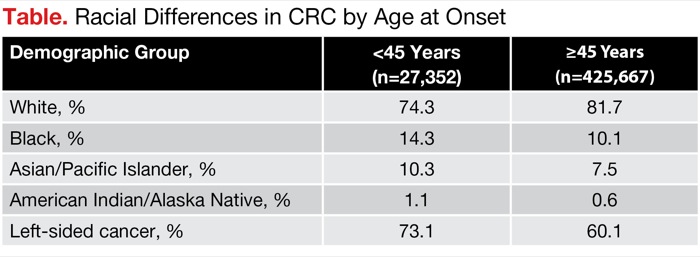
“Clearly, there are risk factors for younger-onset CRC, but more work is required to identify them,” added Dr. Mukhija, who presented the findings at the 2020 GI Cancers Symposium (abstract 62). “With rates of CRC rapidly increasing among young adults, we believe that these demographic differences with racial disparities are important to highlight. As screening programs begin to focus on younger age groups, it will be important to take into account racial differences in CRC in this subgroup so that efforts can be directed toward minority populations [Table].”| Table. Racial Differences in CRC by Age at Onset | ||
| Demographic Group | <45 Years (n=27,352) | ≥45 Years (n=425,667) |
|---|---|---|
| White, % | 74.3 | 81.7 |
| Black, % | 14.3 | 10.1 |
| Asian/Pacific Islander, % | 10.3 | 7.5 |
| American Indian/Alaska Native, % | 1.1 | 0.6 |
| Left-sided cancer, % | 73.1 | 60.1 |
National Cancer Database Analysis
An analysis from the National Cancer Database provided additional insight into racial and sociodemographic disparities in young adults with CRC. In a review of almost 27,000 patients aged 18 to 40 years diagnosed between 2004 and 2016, those with sociodemographic disadvantages had shorter survival than their less disadvantaged peers (abstract 13).
After adjustments for race, stage of cancer, comorbidities and insurance status, people living in areas with low income (<$38,000 annually) and with low educational attainment (high school graduation rate <79%) had a 24% increased risk for death (P=0.004). Compared with living in a major metropolitan region, people in urban or rural areas had a 10% higher risk for death (P=0.02), reported Ashley Matusz-Fisher, MD, a fellow in hematology/oncology at the Levine Cancer Institute, in Charlotte, N.C.
Patients in the low-income, low-education stratum were six times more likely to be black than white and significantly more likely to lack insurance, have comorbidities and have higher pathologic stage at diagnosis, and were less likely to undergo surgery. These characteristics significantly affected survival of all stages, including stage IV disease patients, which was 20.7 months for the disadvantaged group versus 26.1 months for those with higher income and more education (P<0.001), Dr. Matusz-Fisher said.
Limited access to care, lack of awareness of symptoms, and inability to afford necessary treatment may be underlying reasons for these disparities, Dr. Matusz-Fisher said. “To try to eliminate these disparities, the first step is recognition, which is what we are doing, then making people aware of these disparities,” she said.
Mohamed E. Salem, MD, a gastrointestinal oncologist and an associate professor of medicine at Levine Cancer Institute, who led the study, acknowledged that disparities do not necessarily equate with racial or ethnic differences.
“Many other types of disparity exist among our patients, such as age, gender, sexual orientation, disability, literacy level, socioeconomic status and geographic location,” Dr. Salem said. All these factors could affect the availability of and access to cancer care and participation in clinical trials.
“These are aspects that are likely to influence patient outcome and survival,” he said. “Although awareness of health care disparities has increased, considerable knowledge gaps still exist, particularly among young adults with cancer. More effort to increase awareness of health care disparities is warranted in order to provide access and remove barriers to care, particularly for young adults, given the disturbing trend that CRC incidence is on the rise in younger adults.”
How to Mitigate Risk
John M. Carethers, MD, a professor and the chair of internal medicine at the University of Michigan, in Ann Arbor, said social demographics tend to be associated with risk for death from CRC.
“This is true across all ages, even if you equalize these factors in [black] Americans,” Dr. Carethers said. “The question is how to mitigate this and improve outcomes. A large Delaware initiative tackled the problem via screening [J Clin Oncol 2013;31(6):1928-1930]. We don’t typically screen under 50, but for persons over 50, you can essentially eliminate this disparity with navigation services and screening. How do you do that under 50? I’m not quite sure.”
Studies also point to inherent biological differences according to race that may be harder to overcome.
“Data are showing that polyps develop at younger ages and are bigger in certain racial groups, particularly [blacks] and American Indians,” Dr. Carethers said. “You are a victim of your circumstance: living in a low-income area, eating more proinflammatory-type foods, getting your polyps earlier, and then getting your cancers earlier.”
—Clinical Oncology News Staff
Drs. Carethers, Matusz-Fisher and Mukhija reported no relevant financial conflicts of interest.